D185
The future of intraoperative neurophysiological monitoring
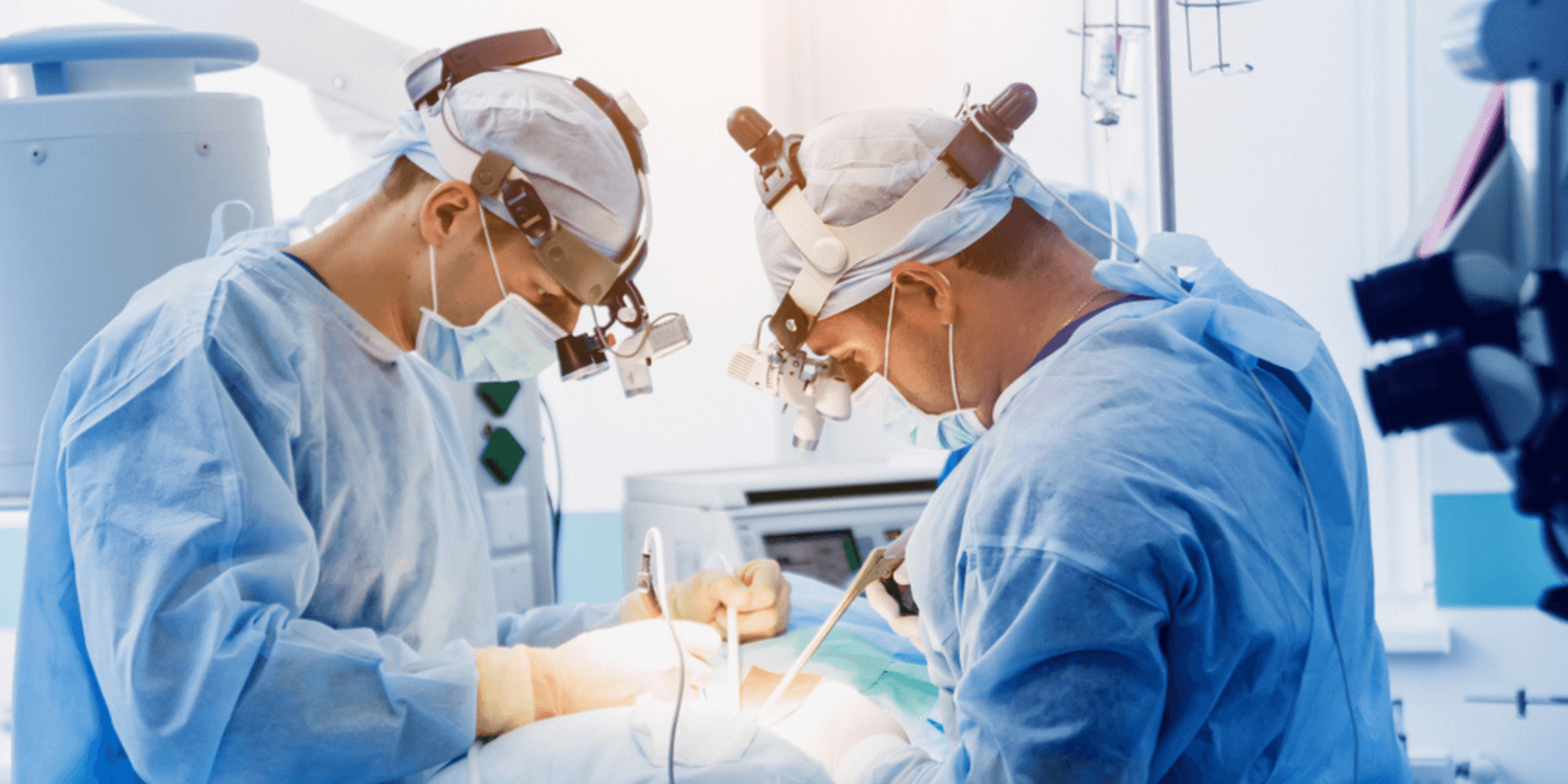
From a slight loss of sensation to complete paraplegia, the reality is, spinal surgical procedures always carry the possibility of causing neurological damage. It’s a risk that’s inherent in their very nature.
That’s why, over the last few decades, surgical teams have used somatosensory evoked potentials (SEPs) as a way to assess spinal cord function during procedures – flagging potential complications and prompting correction, at a stage when it’s still possible to stop or reverse the damage.
There’s no doubt that this type of ‘intraoperative monitoring’ will have protected many patients from surgically-induced neurological deficits. But it’s certainly not without criticism.
Several issues can (and do) arise from using SEPs as a standalone method. Here we take a look at some of these concerns and explore how motor evoked potentials (MEPs) could help.
Common issues with SEPs for intraoperative monitoring
As noted in published peer-reviewed journals.
- Limited scope of monitoring
For anatomical reasons, descending motor fibres may be at greater risk during spinal surgery.
However, whilst SEPs can be used as an indicator of spinal health as a whole, they are mediated primarily by dorsal sensory spinal cord tracts – and are unable to access spinal motor pathways.
As such, these pathways could be independently damaged – without any intraoperative indication.
- Misleading waveforms
On occasion, unchanged SEP waveforms have misled surgeons into continuing with surgery when they shouldn’t have – therefore resulting in unforeseen postoperative neurological complications.
In other cases, SEPs have altered incorrectly – prompting the surgeon to abort the surgical procedure prematurely, only to find the patient has suffered no loss of sensation upon their recovery.
- Consequential delays
SEPs must be averaged, which means they take at least 10-40 seconds to update.
In some situations, this delay can be significant – causing a knock-on effect, whereby it delays warning the surgeon and therefore delays the implementation of any corrective measures.
The consequences of this hold-up can be severe, leading to irreversible neurological damage.
- Reliability
As SEPs are generally small in magnitude, they can also be difficult to monitor reliably in some patients – particularly those presenting with pre-existing neuropathies.
Could MEPs be the solution?
Due to the issues highlighted above, intraoperative monitoring with MEPs (rather than SEPs) has become an increasingly popular option among surgeons.
Essentially, MEPs are conducted down the spinal cord – by stimulating the motor cortex of the brain transcranially with high-frequency trains of stimuli. These can then be easily recorded from the muscles, providing a good indication of the integrity of the spinal motor pathways.
These are the same pathways used by the brain to trigger and control voluntary movement. Therefore, any alterations in the MEP waveforms can provide the surgical team with a crucial warning of possible complications and the need to act to prevent these.

MEPs offer a number of advantages over traditional SEPs. For example, they:
- allow the whole of the motor system to be exclusively monitored
- offer greater accuracy for motor outcomes (than SEPs do for sensory outcomes), reliably indicating whether it’s safe to continue with a procedure
- facilitate real-time updates, therefore preventing any delays to corrective measures
- assess the upper and lower limbs independently
- minimise patient discomfort
As a result, the application of motor evoked potential monitoring is rapidly expanding in neurosurgery and is now used for a wide range of procedures – including the removal of spinal cord tumours, correction of scoliosis, cervical spine surgery, thoraco-abdominal aortic aneurysm repair and more.
Digitimer – pioneers in MEP monitoring
Considering a switch to MEP monitoring?
Developed as part of our human neurophysiology range, the D185 MultiPulse Transcranial Cortical Stimulator was the first – and remains the only standalone surgical stimulator with FDA clearance for this technique.
Primarily, it is intended for the intraoperative monitoring of spinal motor pathways. And as a testament to its capabilities, the D185 is now used by neurosurgeons and cardiovascular surgeons all over the world for this purpose – both as a standalone method and in conjunction with SEPs.
Thanks to its 1000V power source, the device can even generate MEPs in patients with pre-existing neuropathies – therefore adding to its accuracy and reliability.
In addition, the D185 stimulator can also be a useful tool for peripheral nerve stimulation and is frequently used by medics in the diagnosis of peripheral nerve disorders, such as multifocal motor neuropathy and motor neurone disease.
Interested in learning more?
For further information on our pioneering transcranial stimulator and how it can be used for intraoperative neurophysiological monitoring, be sure to take a look at our product brochure and supporting product documents. These feature additional technical information and detailed specifications that should be able to help.
You’re also welcome to contact us at any time.
We’re always happy to assist with your enquiry and will gladly talk you through the features of the D185 and how it could be of benefit to your surgical team. Simply give us a call on +44 (0)1707 328347 or send an email to [email protected].
Alternatively, if you’d like to register your interest in the D185 and request a quote, you can do so by filling out our online form. A member of the team will respond as soon as possible.